Tumor Mutational Burden (TMB)

Tumor Mutational Burden (TMB): Overview and Clinical Implications
Tumor Mutational Burden (TMB) quantifies the number of non-inherited somatic mutations per megabase (Mb) of tumor DNA. It serves as a predictive and prognostic biomarker in oncology, particularly for immunotherapy response. Below is a synthesis of its key aspects, supported by current evidence.
Key Features of TMB
Definition:
- TMB measures somatic mutations (coding region changes) in tumor DNA, excluding germline mutations.
- Expressed as mutations per megabase (mut/Mb).
Mechanism:
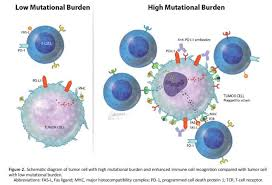
- High TMB correlates with increased neoantigen production, enhancing immune recognition via cytotoxic T-cells.
- Immune checkpoint inhibitors (ICIs) amplify this response by blocking regulatory pathways (e.g., PD-1/PD-L1).
Clinical Applications
Immunotherapy Prediction:
- FDA Approval: Pembrolizumab is approved for advanced solid tumors with TMB-High (≥10 mut/Mb) after progression on prior therapies[1][2][5].
- Response Correlation: TMB-High tumors (e.g., melanoma, NSCLC) show improved survival with ICIs[3][6].
Prognostic Value:
- Mixed Outcomes:
- Cervical Cancer: High TMB predicts worse survival post-radiotherapy, suggesting context-dependent utility[4].
- Colorectal Cancer: TMB-High (>20 mut/Mb) linked to microsatellite instability (MSI-High), indicating immunotherapy candidacy[3].
Measurement and Challenges
Testing Methods:
- Next-Generation Sequencing (NGS):
- Whole Exome Sequencing (WES): Gold standard but costly.
- Targeted Panels: Require ≥1.1 Mb coverage for accuracy (e.g., Illumina, Caris Life Sciences)[6][7][8].
- Emerging Techniques: Blood-based TMB (bTMB) via circulating tumor DNA (ctDNA)[3][8].
Standardization Issues:
- Variability: Panel size, gene coverage, and bioinformatics pipelines affect TMB estimates[2][7].
- Thresholds:
- TMB-Low: 10–20 mut/Mb (varies by cancer type)[3][8].
Limitations and Research Directions
Context-Dependent Utility:
- Predictive power varies by cancer type (e.g., limited in prostate/pancreatic cancers)[2][5].
- Combination Biomarkers: Integration with MSI, PD-L1, or neoantigen clonality improves accuracy[2][5][8].
Conflicting Evidence:
- Radiotherapy: High TMB may indicate poor prognosis in cervical cancer, contrasting with ICI benefits[4].
Future Directions
- Standardization: Harmonizing TMB calculation across platforms[7].
- Liquid Biopsies: Validating bTMB for non-invasive monitoring[3][8].
- Comprehensive Genomic Profiling (CGP): Capturing TMB, MSI, and actionable mutations in one assay[8].
Conclusion
TMB is a dynamic biomarker guiding immunotherapy decisions but requires context-specific interpretation. While TMB-High tumors often respond better to ICIs, its prognostic value varies by treatment modality and cancer type. Standardization and multimodal biomarker integration are critical for optimizing clinical utility.
Consult with Our Team of Experts Now!
At DrStemCellsThailand (DRSCT)‘s Anti-Aging and Regenerative Medicine Center of Thailand, we emphasize comprehensive evaluations and personalized treatment plans of Cellular Therapy and Stem Cells for managing various health conditions. If you have questions about Tumor Mutational Burden (TMB) or would like more information on our services, consult with our experts today!
Consult with Our Team of Experts Now!
References