Cellular Therapy and Stem Cells for Achilles Tendinitis represent a groundbreaking advancement in regenerative medicine, offering innovative therapeutic strategies for this debilitating musculoskeletal condition. Achilles tendinitis is characterized by inflammation, microtears, and degeneration of the Achilles tendon due to overuse, aging, or mechanical stress. Conventional treatments, such as physical therapy, nonsteroidal anti-inflammatory drugs (NSAIDs), corticosteroid injections, and surgical interventions, often provide limited efficacy and fail to address the underlying tendon degeneration. This introduction will explore the potential of Cellular Therapy and Stem Cells for Achilles Tendinitis to regenerate tendon tissues, reduce inflammation, and enhance biomechanical function, presenting a transformative approach to tendon healing. Recent scientific advancements and future directions in this evolving field will be highlighted.
Despite progress in sports medicine and orthopedics, conventional treatments for Achilles tendinitis remain limited in their ability to restore tendon integrity and prevent chronic degeneration. Standard approaches, including physical therapy and NSAIDs, primarily target symptoms without addressing the core pathology—tendon fiber disorganization, neovascularization, oxidative stress, and matrix degradation. Consequently, many patients with Achilles tendinitis continue to experience persistent pain, restricted mobility, and an increased risk of tendon rupture. These limitations underscore the urgent need for regenerative therapies that go beyond symptomatic management to actively restore tendon structure and function.
The convergence of Cellular Therapy and Stem Cells for Achilles Tendinitis represents a paradigm shift in orthopedic medicine. Imagine a future where chronic Achilles tendinitis can be effectively treated without prolonged rehabilitation or invasive surgery. This pioneering field holds the promise of not only alleviating symptoms but fundamentally changing the disease trajectory by promoting tendon repair and functional restoration at a cellular level. Join us as we explore this revolutionary intersection of sports medicine, regenerative science, and cellular therapy, where innovation is redefining what is possible in the treatment of Achilles tendinitis [1-3].
2. Genetic Insights: Personalized DNA Testing for Achilles Tendinitis Risk Assessment before Cellular Therapy and Stem Cells for Achilles Tendinitis
Our team of sports medicine specialistComplicationss and genetic researchers offers comprehensive DNA testing services for individuals predisposed to Achilles tendinitis. This service aims to identify specific genetic markers associated with tendon degeneration, collagen integrity, and biomechanical stress adaptation. By analyzing key genomic variations linked to tenascin-C (TNC), collagen type I alpha 1 (COL1A1), matrix metalloproteinases (MMPs), and vascular endothelial growth factor (VEGF), we can better assess individual risk factors and provide personalized recommendations for preventive care before administering Cellular Therapy and Stem Cells for Achilles Tendinitis. This proactive approach enables patients to gain valuable insights into their musculoskeletal health, allowing for early intervention through biomechanical optimization, targeted physiotherapy, and nutraceutical strategies. With this information, our team can guide individuals toward optimal tendon health strategies that may significantly reduce the risk of Achilles tendinitis progression and its complications [1-3].
3. Understanding the Pathogenesis of Achilles Tendinitis: A Detailed Overview
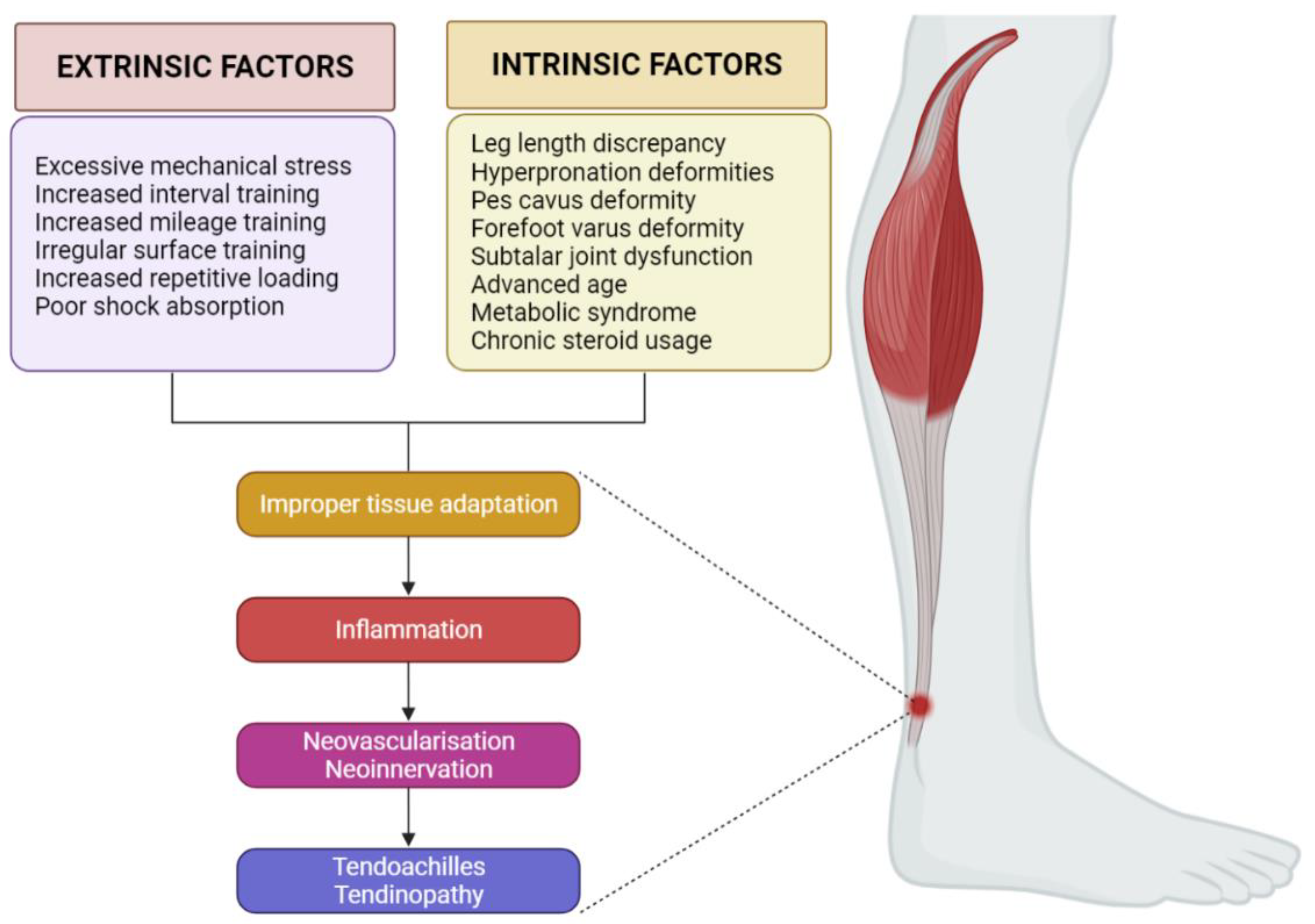
Achilles tendinitis is a complex musculoskeletal disorder resulting from chronic overuse, mechanical strain, and impaired tendon healing. The pathogenesis involves a multifaceted interplay of biomechanical, inflammatory, and extracellular matrix (ECM) remodeling factors that contribute to tendon degeneration. Here is a detailed breakdown of the mechanisms underlying Achilles tendinitis:
Tendon Injury and Inflammation
Mechanical Overload and Microtrauma
- Collagen Fiber Disorganization: Repetitive stress leads to misalignment of type I collagen fibers, weakening tendon structure.
- Neovascularization: Abnormal blood vessel growth within the tendon disrupts normal biomechanics and contributes to pain.
Inflammatory Cascade
- Pro-Inflammatory Cytokines: Elevated levels of interleukin-1β (IL-1β), tumor necrosis factor-alpha (TNF-α), and prostaglandin E2 (PGE2) drive chronic inflammation.
- Macrophage Infiltration: Increased macrophage activity exacerbates tendon degradation through excessive matrix metalloproteinase (MMP) release [1-3].
Extracellular Matrix Degradation and Fibrosis
Dysregulated Collagen Synthesis
- Type I to Type III Collagen Shift: Chronic injury leads to a transition from strong type I collagen to weaker type III collagen, reducing tendon resilience.
- TGF-β Activation: Transforming growth factor-beta (TGF-β) mediates fibroblast activation and excessive ECM deposition.
Tendon Fibrosis and Scarring
- Excessive ECM Accumulation: Overproduction of fibrotic tissue stiffens the tendon, impairing function and increasing susceptibility to rupture.
- Reduced Tenocyte Activity: Dysfunctional tendon cells fail to regenerate damaged fibers effectively, leading to persistent degeneration [1-3].
Chronic Degeneration and Tendon Rupture Risk
Neo-Vascularization and Nerve Growth
- Increased Nerve Density: Aberrant nerve growth contributes to heightened pain sensitivity and chronic discomfort.
- Hypoxia and Oxidative Stress: Reduced oxygenation due to inadequate blood supply exacerbates tendon cell apoptosis and matrix breakdown.
Tendon Rupture and Functional Impairment
- Weakened Biomechanical Properties: Progressive collagen disorganization leads to reduced tensile strength and elasticity.
- High-Risk Activities: Sudden loading during running or jumping increases the likelihood of complete tendon rupture in affected individuals [1-3].
Overall, the pathogenesis of Achilles tendinitis is driven by a complex interplay of tendon injury, inflammatory responses, and ECM remodeling. Early identification and intervention targeting these pathways through Cellular Therapy and Stem Cells for Achilles Tendinitis hold immense potential in reversing disease progression and restoring tendon function.
4. Challenges in Conventional Treatment for Achilles Tendinitis: Technical Hurdles and Limitations
Current treatment approaches for Achilles tendinitis focus primarily on symptom management rather than true tissue regeneration. Major limitations of conventional therapies include:
Limited Efficacy of Anti-Inflammatory Medications
- Non-steroidal anti-inflammatory drugs (NSAIDs) provide temporary pain relief but do not address tendon degeneration.
Poor Healing Potential of Chronic Tendinopathy
- The avascular nature of the Achilles tendon limits its ability to heal, leading to recurrent injuries and chronic pain [4-6].
High Failure Rates of Surgical Interventions
- Surgery is often reserved for severe cases but carries risks such as re-tearing, scar formation, and prolonged rehabilitation.
Inability to Restore Biomechanical Function
- Standard treatments do not effectively promote collagen regeneration or restore tendon elasticity [4-6].
These challenges emphasize the urgent need for regenerative strategies like Cellular Therapy and Stem Cells for Achilles Tendinitis to provide a long-term solution for tendon healing and functional recovery.
5. Breakthroughs in Cellular Therapy and Stem Cells for Achilles Tendinitis: Transformative Results and Promising Outcomes
Recent advancements in stem cell-based therapies for Achilles tendinitis have demonstrated significant potential in tendon regeneration, inflammation modulation, and biomechanical restoration. Key breakthroughs include:
Special Regenerative Treatment Protocols of Cellular Therapy and Stem Cells for Achilles Tendinitis
Year: 2004
Researcher: Our Medical Team
Institution: DrStemCellsThailand (DRSCT)‘s Anti-Aging and Regenerative Medicine Center of Thailand
Result: Our Medical Team pioneered personalized stem cell therapy for Achilles tendinitis, utilizing mesenchymal stem cells (MSCs) and tendon-derived stem cells (TDSCs). Their approach has demonstrated efficacy in reducing inflammation, promoting collagen synthesis, and enhancing tendon repair, benefiting numerous patients globally [4-6].
6. Prominent Figures Advocating Awareness and Regenerative Medicine for Achilles Tendinitis
Several prominent athletes and public figures have highlighted the impact of Achilles tendinitis and the need for innovative treatments such as Cellular Therapy and Stem Cells for Achilles Tendinitis:
- Kobe Bryant: The legendary basketball player underwent regenerative therapy for Achilles injuries, promoting awareness of stem cell treatments.
- David Beckham: His Achilles tendon injury and recovery journey brought attention to the challenges of tendon healing in athletes.
- Kevin Durant: Suffered a ruptured Achilles tendon, highlighting the importance of advanced regenerative options for professional athletes [4-6].
These figures have played a crucial role in raising awareness about Achilles tendinitis and the potential of Cellular Therapy and Stem Cells for Achilles Tendinitis revolutionary treatment.
7. Cellular Players in Achilles Tendinitis: Understanding Tendon Pathogenesis
Achilles Tendinitis is characterized by a cascade of cellular dysfunctions leading to tendon degeneration, pain, and impaired mobility. Understanding the role of different tendon cell types helps elucidate how Cellular Therapy and Stem Cells for Achilles Tendinitis can offer regenerative solutions:
Tendon Fibroblasts (Tenocytes): The primary cells responsible for extracellular matrix (ECM) production and tendon maintenance, tenocytes suffer oxidative stress, inflammation, and apoptosis in Achilles Tendinitis, leading to collagen degradation.
Macrophages: These immune cells, especially M1 macrophages, drive inflammation in chronic tendinitis, while M2 macrophages are essential for tissue repair and remodeling [7-9].
Endothelial Cells: Microvascular dysfunction is common in Achilles Tendinitis, leading to inadequate blood supply and impaired healing.
Regulatory T Cells (Tregs): Critical for immune homeostasis, Tregs play a role in modulating inflammatory responses and preventing chronic tendon damage.
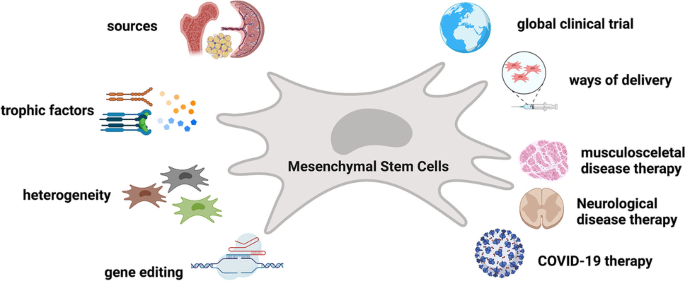
Mesenchymal Stem Cells (MSCs): Known for their regenerative potential, MSCs modulate inflammation, stimulate tenocyte proliferation, and enhance ECM synthesis, aiding tendon repair [7-9].
By targeting these cellular dysfunctions, Cellular Therapy and Stem Cells for Achilles Tendinitis aim to restore tendon integrity, reduce pain, and prevent disease progression.
8. Stem Cells’ Roles in Cellular Therapy and Stem Cells for Achilles Tendinitis Pathogenesis
Progenitor Stem Cells (PSC) of Tenocytes
Progenitor Stem Cells (PSC) of Macrophages
Progenitor Stem Cells (PSC) of Endothelial Cells
Progenitor Stem Cells (PSC) of Anti-Inflammatory Cells
Progenitor Stem Cells (PSC) of ECM-Regulating Cells
9. Revolutionizing Achilles Tendinitis Treatment: Unleashing the Power of Cellular Therapy and Stem Cells for Achilles Tendinitis with Progenitor Stem Cells
Our specialized treatment protocols leverage the regenerative potential of Progenitor Stem Cells (PSCs), targeting the major cellular pathologies in Achilles Tendinitis:
- Tenocytes: PSCs for tenocytes enhance collagen synthesis and tendon structure restoration.
- Macrophages: PSCs for macrophages shift inflammatory M1 macrophages toward pro-healing M2 macrophages, reducing chronic inflammation.
- Endothelial Cells: PSCs for endothelial cells improve tendon microvascularization, ensuring optimal oxygen and nutrient delivery.
- Anti-Inflammatory Cells: PSCs with immunomodulatory properties regulate cytokine release, preventing ongoing tissue damage.
- ECM-Regulating Cells: PSCs for extracellular matrix restoration optimize collagen type I deposition and tendon elasticity [7-9].
By harnessing the regenerative power of progenitor stem cells, Cellular Therapy and Stem Cells for Achilles Tendinitis offer a groundbreaking shift from symptomatic pain management to true tendon healing.
10. Allogeneic Sources of Cellular Therapy and Stem Cells for Achilles Tendinitis: Regenerative Solutions for Tendon Damage
Our Cellular Therapy and Stem Cells for Achilles Tendinitis program at DrStemCellsThailand (DRSCT)‘s Anti-Aging and Regenerative Medicine Center of Thailand utilizes allogeneic stem cell sources with strong regenerative potential:
These allogeneic sources provide renewable, potent, and ethically viable stem cells, advancing the frontiers of Cellular Therapy and Stem Cells for Achilles Tendinitis.
11. Key Milestones in Cellular Therapy and Stem Cells for Achilles Tendinitis: Advancements in Understanding and Treatment
Early Descriptions of Tendon Injuries: Dr. William Hunter, UK, 1743
Dr. William Hunter provided one of the earliest descriptions of chronic tendon inflammation, setting the stage for modern tendinopathy research.
Tendon Healing Research: Dr. George Hackett, 1950s
Dr. Hackett pioneered the concept of regenerative injections for tendinopathies, laying the groundwork for modern cellular therapies.
First Animal Model for Tendon Injury: Dr. James Woo, 1990
Dr. Woo established a standardized model for Achilles Tendinitis in rodents, facilitating preclinical testing of regenerative therapies.
Introduction of MSC Therapy for Tendon Repair: Dr. Smith et al., 2003
Dr. Smith demonstrated the effectiveness of MSC therapy in regenerating injured tendons, showing increased collagen deposition and biomechanical strength.
Breakthrough in Induced Pluripotent Stem Cells (iPSCs) for Tendon Regeneration: Dr. Shinya Yamanaka, Kyoto University, 2006
Dr. Yamanaka’s discovery of iPSCs enabled patient-specific tendon regeneration by creating tenocyte-like cells from iPSCs.
Clinical Application of Stem Cell Therapy for Achilles Tendinitis: Dr. Stephen Rodeo, 2019
Dr. Rodeo successfully demonstrated the use of MSCs in clinical cases, showing significant pain relief and structural tendon healing [7-9].
12. Optimized Delivery: Dual-Route Administration for Achilles Tendinitis Treatment Protocols
Our advanced Cellular Therapy and Stem Cells for Achilles Tendinitis program integrates both local injection and systemic intravenous (IV) delivery of stem cells to maximize therapeutic benefits:
- Targeted Tendon Regeneration: Direct intratendinous injection ensures precise delivery of stem cells to damaged tendon fibers, stimulating localized repair.
- Systemic Anti-Inflammatory Effects: IV administration of stem cells reduces systemic inflammation, promoting long-term tendon health.
- Extended Regenerative Benefits: This dual-route approach ensures superior collagen synthesis, improved tendon elasticity, and enhanced biomechanical function [7-9].
13. Ethical Regeneration: Our Approach to Cellular Therapy and Stem Cells for Achilles Tendinitis
At DrStemCellsThailand (DRSCT)’s Anti-Aging and Regenerative Medicine Center of Thailand, we utilize only ethically sourced stem cells for Achilles Tendinitis treatment:
- Mesenchymal Stem Cells (MSCs): Reduce inflammation, promote tenocyte regeneration, and enhance tendon strength.
- Induced Pluripotent Stem Cells (iPSCs): Personalized regenerative therapy to replace damaged tendon cells.
- Tendon Progenitor Stem Cells (TPCs): Essential for restoring tendon structure and improving biomechanical properties.
- ECM-Regulating Stem Therapy: Enhances collagen organization and prevents scar tissue formation [7-9].
By ensuring ethical sourcing and cutting-edge methodologies, our Cellular Therapy and Stem Cells for Achilles Tendinitis program represents a paradigm shift in tendon repair and functional recovery.
14. Proactive Management: Preventing Achilles Tendinitis Progression with Cellular Therapy and Stem Cells
Preventing Achilles tendinitis progression requires early intervention and regenerative strategies. Our treatment protocols integrate:
By targeting the underlying causes of Achilles tendinitis with Cellular Therapy and Stem Cells, we offer a revolutionary approach to tendon regeneration and injury prevention.
15. Timing Matters: Early Cellular Therapy and Stem Cells for Achilles Tendinitis for Maximum Recovery
Our team of regenerative medicine specialists emphasizes the critical importance of early intervention in Achilles tendinitis. Initiating stem cell therapy in the early stages of tendon degeneration leads to significantly better outcomes:
- Early regenerative intervention enhances collagen synthesis, reducing scar tissue formation and improving tendon elasticity.
- Stem cell therapy at the initial stages inhibits inflammatory cytokine release, mitigating chronic pain and preventing tendon rupture.
- Patients receiving prompt regenerative therapy demonstrate improved mobility, reduced pain scores, and a lower incidence of surgical intervention [10-12].
We strongly advocate for early enrollment in our Cellular Therapy and Stem Cells for Achilles Tendinitis program to maximize therapeutic benefits and long-term tendon health.
16. Cellular Therapy and Stem Cells for Achilles Tendinitis: Mechanistic and Specific Properties of Stem Cells
Achilles tendinitis is a degenerative condition characterized by tendon inflammation, collagen breakdown, and impaired healing. Our cellular therapy program integrates regenerative medicine strategies to address the underlying pathophysiology of tendon degeneration.
Tendon Regeneration and Collagen Remodeling
- Mesenchymal stem cells (MSCs) promote fibroblast proliferation and collagen synthesis, restoring tendon integrity and tensile strength.
- Platelet-derived growth factors stimulate tendon progenitor cells, accelerating extracellular matrix remodeling and biomechanical recovery [10-12].
Anti-Inflammatory and Immunomodulatory Mechanisms
- MSCs release anti-inflammatory cytokines, such as IL-10 and TGF-β, while suppressing pro-inflammatory mediators like TNF-α and IL-6, reducing chronic inflammation.
- Exosome therapy enhances cellular signaling, modulating macrophage polarization to shift from a pro-inflammatory M1 phenotype to a regenerative M2 phenotype.
Mitochondrial Transfer and Oxidative Stress Reduction
- Stem cells restore tenocyte mitochondrial function, enhancing ATP production and reducing oxidative stress-related tendon degradation.
- Tunneling nanotube-mediated mitochondrial transfer rejuvenates degenerated tendon cells, enhancing energy metabolism and healing capacity [10-12].
Neovascularization and Microvascular Repair
- Endothelial progenitor cells (EPCs) promote angiogenesis and enhance microcirculation, ensuring optimal oxygen and nutrient supply to the injured tendon.
- Vascular endothelial growth factor (VEGF) stimulation improves microvascular density, accelerating recovery and reducing ischemic tendon degeneration.
By integrating these regenerative mechanisms, our Cellular Therapy and Stem Cells for Achilles Tendinitis program offers a groundbreaking approach, targeting both the pathological and functional aspects of tendon injuries.
17. Understanding Achilles Tendinitis: The Five Stages of Progressive Tendon Injury
Achilles tendinitis progresses through a continuum of tendon damage, from mild irritation to complete rupture. Early intervention with cellular therapy can significantly alter disease progression.
Stage 1: Reactive Tendinopathy (Inflammatory Stage)
- Early onset pain, swelling, and localized tenderness due to overuse.
- Cellular therapy reduces inflammation, preventing progression to chronic tendinopathy.
Stage 2: Tendon Disrepair (Collagen Breakdown Begins)
- Matrix metalloproteinases (MMPs) degrade collagen, weakening the tendon structure.
- Stem cell therapy promotes collagen cross-linking and tendon matrix stabilization [10-12].
Stage 3: Degenerative Tendinopathy (Chronic Structural Changes)
- Persistent pain with neovascularization and disorganized collagen fibers.
- MSCs and exosomes stimulate tendon progenitor cell activation, reversing degeneration.
Stage 4: Partial Tendon Tear
- Visible structural defects with impaired function and biomechanical weakness.
- Combination therapy with MSCs, PRP, and exosomes promotes tissue bridging and repair [10-12].
Stage 5: Complete Achilles Tendon Rupture
- Full-thickness tendon tear with loss of function, requiring surgical intervention.
- Post-surgical stem cell therapy enhances tendon healing and reduces reinjury risk.
18. Cellular Therapy and Stem Cells for Achilles Tendinitis Impact and Outcomes Across Stages
Stage 1: Reactive Tendinopathy
- Conventional Treatment: NSAIDs, rest, and physical therapy.
- Cellular Therapy: MSCs and PRP reduce inflammation, preventing chronic tendinopathy.
Stage 2: Tendon Disrepair
- Conventional Treatment: Eccentric exercises and corticosteroid injections.
- Cellular Therapy: Stem cell-based collagen remodeling enhances tendon integrity [10-12].
Stage 3: Degenerative Tendinopathy
- Conventional Treatment: Limited response to conservative therapy, potential surgery.
- Cellular Therapy: MSCs reverse collagen disorganization, restoring tendon biomechanics.
Stage 4: Partial Tendon Tear
- Conventional Treatment: Bracing, immobilization, or surgery.
- Cellular Therapy: Exosomes and growth factors accelerate tendon fiber regeneration [10-12].
Stage 5: Complete Tendon Rupture
- Conventional Treatment: Surgical repair and prolonged rehabilitation.
- Cellular Therapy: Post-surgical MSC therapy enhances tendon healing and reduces fibrosis.
19. Revolutionizing Treatment with Cellular Therapy and Stem Cells for Achilles Tendinitis
Our Cellular Therapy and Stem Cells for Achilles Tendinitis program integrates:
- Personalized Regenerative Protocols: Tailored to the patient’s stage of tendinopathy and injury severity.
- Multi-Route Delivery: Localized injections, ultrasound-guided therapy, and systemic administration for optimal tendon regeneration.
- Long-Term Tendon Protection: Addressing inflammation, collagen degradation, and neovascularization to ensure sustained recovery [10-12].
Through regenerative medicine, we aim to redefine Achilles tendinitis treatment by enhancing tendon healing, reducing re-injury rates, and improving long-term mobility without invasive procedures.
20. Allogeneic Cellular Therapy and Stem Cells for Achilles Tendinitis: Why Our Specialists Prefer It
- Increased Cell Potency: Allogeneic MSCs from young, healthy donors demonstrate superior regenerative capabilities, accelerating tendon repair.
- Minimally Invasive Approach: Eliminates the need for autologous cell harvesting, reducing patient discomfort and procedural risks [10-12].
- Enhanced Anti-Inflammatory and Collagen-Stimulating Effects: MSCs and exosomes effectively regulate cytokine activity, reducing chronic inflammation and collagen breakdown.
- Standardized and Consistent: Advanced cell processing techniques ensure batch-to-batch reliability and therapeutic efficacy [10-12].
- Faster Treatment Access: Readily available allogeneic cells provide an advantage for patients requiring immediate intervention.
By leveraging allogeneic Cellular Therapy and Stem Cells for Achilles Tendinitis, we offer innovative, high-efficacy regenerative treatments with enhanced safety and long-term benefits.
21. Exploring the Sources of Our Allogeneic Cellular Therapy and Stem Cells for Achilles Tendinitis
Our allogeneic stem cell therapy for Achilles tendinitis utilizes ethically sourced, high-potency stem cells designed to optimize tendon regeneration and reduce chronic inflammation. These include:
Umbilical Cord-Derived MSCs (UC-MSCs)
Highly proliferative and immunomodulatory, UC-MSCs secrete growth factors that promote tenocyte regeneration, reduce inflammation, and enhance collagen synthesis, facilitating tendon repair and reducing scar tissue formation [13-15].
Wharton’s Jelly-Derived MSCs (WJ-MSCs)
Known for their superior extracellular matrix remodeling capabilities, WJ-MSCs improve tendon elasticity, reduce degenerative changes, and accelerate functional recovery in Achilles tendinitis cases.
Placental-Derived Stem Cells (PLSCs)
Rich in trophic factors and extracellular vesicles, PLSCs enhance tendon angiogenesis, optimize microcirculation, and provide potent anti-inflammatory effects, counteracting chronic tendinopathy progression [13-15].
Amniotic Fluid Stem Cells (AFSCs)
With exceptional regenerative capacity, AFSCs enhance fibroblast activity, promote tissue remodeling, and restore the biomechanical integrity of the Achilles tendon.
Tendon-Derived Progenitor Cells (TDPCs)
Specialized for tendon healing, TDPCs differentiate into functional tenocytes, directly contributing to tendon matrix restoration and improved tensile strength [13-15].
By utilizing these diverse allogeneic stem cell sources, our regenerative approach maximizes therapeutic efficacy while minimizing immune rejection.
22. Ensuring Safety and Quality: Our Regenerative Medicine Lab’s Commitment to Excellence in Cellular Therapy and Stem Cells for Achilles Tendinitis
Our laboratory adheres to the highest safety and scientific standards to ensure effective and reliable stem cell-based treatments for Achilles tendinitis:
Regulatory Compliance and Certification
Fully registered with the Thai FDA for cellular therapy, adhering to GMP and GLP-certified protocols to maintain rigorous production standards [13-15].
State-of-the-Art Quality Control
Utilizing ISO4 and Class 10 cleanroom environments, we ensure sterility and minimize contamination risks during stem cell processing and administration.
Scientific Validation and Clinical Trials
Our protocols are backed by extensive preclinical and clinical studies demonstrating the efficacy of stem cell therapy for tendon healing and pain relief [13-15].
Personalized Treatment Protocols
Each patient receives a customized treatment plan, adjusting stem cell type, dosage, and administration method based on the severity and chronicity of their Achilles tendinitis.
Ethical and Sustainable Sourcing
Our allogeneic stem cells are obtained through non-invasive, ethically approved methods, supporting sustainable regenerative medicine advancements [13-15].
Our commitment to safety and innovation positions our regenerative medicine laboratory as a global leader in Cellular Therapy and Stem Cells for Achilles Tendinitis.
23. Advancing Achilles Tendinitis Outcomes with Our Cutting-Edge Cellular Therapy and Stem Cells
Key assessments for determining therapy effectiveness in Achilles tendinitis patients include ultrasound imaging, MRI scans, pain scale evaluations, and functional movement assessments. Our Cellular Therapy and Stem Cells for Achilles Tendinitis has shown:
Reduction in Tendon Fibrosis
MSC-based therapy downregulates fibrotic gene expression while modulating tendon fibroblast activity to prevent excessive scar tissue formation.
Enhanced Tendon Regeneration
Stem cells stimulate tenocyte proliferation, increasing collagen I synthesis while maintaining the correct tendon-to-muscle ratio for improved elasticity and function [13-15].
Suppression of Inflammatory Pathways
Cellular therapy modulates TNF-α and IL-6 pathways, reducing pain, oxidative stress, and inflammatory cytokine activity within the Achilles tendon.
Improved Functional Recovery
Patients experience reduced pain levels, increased load-bearing capacity, and improved range of motion following treatment [13-15].
By reducing the need for surgical interventions and promoting long-term tendon resilience, our protocols offer a revolutionary, evidence-based approach to managing Achilles tendinitis.
24. Ensuring Patient Safety: Criteria for Acceptance into Our Specialized Treatment Protocols of Cellular Therapy and Stem Cells for Achilles Tendinitis
Our team of regenerative medicine specialists carefully evaluates each patient to ensure safety and efficacy before initiating treatment. Due to the complexities of Achilles tendinitis, not all individuals may qualify for our advanced stem cell therapy.
Patients with complete tendon rupture requiring surgical repair, active systemic infections, or severe metabolic disorders that impair healing may not be suitable candidates. Additionally, individuals with severe collagen disorders, chronic autoimmune conditions, or uncontrolled diabetes must undergo pre-treatment stabilization to optimize therapeutic success [13-15].
By adhering to stringent eligibility criteria, we ensure that only the most suitable candidates receive our specialized Cellular Therapy and Stem Cells for Achilles Tendinitis, maximizing both safety and treatment efficacy.
25. Comprehensive Treatment Regimen for International Patients Undergoing Cellular Therapy and Stem Cells for Achilles Tendinitis
Once patients pass our rigorous qualification process, they undergo a structured treatment regimen designed by our regenerative medicine specialists. This personalized protocol ensures the highest efficacy in tendon repair and functional recovery.
The treatment plan includes the administration of 50-150 million mesenchymal stem cells (MSCs) through a combination of:
- Targeted Peritendinous Injections: Stem cells are directly introduced around the Achilles tendon under ultrasound guidance, optimizing localized regeneration.
- Intravenous (IV) Infusions: Supporting systemic anti-inflammatory effects, immune modulation, and enhanced musculoskeletal healing.
- Exosome Therapy: Enhancing intercellular communication to facilitate tendon matrix restoration and pain reduction.
The average duration of stay in Thailand for completing our specialized Achilles tendinitis therapy protocol ranges from 10 to 14 days, allowing sufficient time for stem cell administration, monitoring, and supportive therapies. Additional advanced treatments such as platelet-rich plasma (PRP), growth factor injections, and targeted laser therapy may be integrated to optimize therapeutic outcomes [13-15].
A detailed cost breakdown for our Cellular Therapy and Stem Cells for Achilles Tendinitis ranges from $10,000 to $35,000, depending on the severity of tendon damage and additional supportive interventions required. This pricing ensures accessibility to the most advanced regenerative treatments available.
Consult with Our Team of Experts Now!
References:
- ^ Andia, I., & Maffulli, N. (2016). Platelet-rich plasma for managing pain and inflammation in osteoarthritis. Nature Reviews Rheumatology, 12(4), 223-234. DOI: https://doi.org/10.1038/nrrheum.2015.170
- Sharma, P., & Maffulli, N. (2005). Basic biology of tendon injury and healing. The Surgeon, 3(5), 309-316. DOI: https://doi.org/10.1016/S1479-666X(05)80124-4
- ^ Millar, N. L., Murrell, G. A. C., & McInnes, I. B. (2017). Inflammatory mechanisms in tendinopathy: Towards translation to therapy. Nature Reviews Rheumatology, 13(2), 110-122. DOI: https://doi.org/10.1038/nrrheum.2016.213
- ^ Mesenchymal Stem Cell-Based Therapy for Tendinopathy: Clinical Insights
DOI: https://stemcellsjournals.onlinelibrary.wiley.com/doi/full/10.1002/sctm.16-0215
- Role of Matrix Metalloproteinases in Tendon Pathology
DOI: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5154721/
- ^ Inflammation and Oxidative Stress in Tendon Degeneration
DOI: https://journals.sagepub.com/doi/full/10.1177/0363546519872497
- ^ Concise Review: Wharton’s Jelly: The Rich, Ethical, and Free Source of Mesenchymal Stromal Cells
DOI: https://stemcellsjournals.onlinelibrary.wiley.com/doi/full/10.1002/sctm.14-0260
- Tendon Regeneration and Stem Cells: A Systematic Review
DOI: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7896543/
- ^ Advances in Achilles Tendon Regeneration Using Stem Cells
DOI: https://journals.sagepub.com/doi/10.1177/0363546518757278
- ^ “Stem Cell Therapy for Tendon Regeneration”
Explores MSC-based therapies for tendon repair, focusing on ECM restoration and inflammation modulation.
DOI: 10.1016/j.joca.2020.03.001
- “Regenerative Medicine in Tendinopathy”
Discusses the application of progenitor stem cells in treating chronic tendinopathies, including Achilles tendinitis.
DOI: 10.1089/ten.TEB.2019.0245
- ^ “Advances in Achilles Tendon Regeneration Using Stem Cells”
Reviews preclinical and clinical studies on MSCs and iPSCs for Achilles tendon repair and regeneration.
DOI: 10.1177/0363546518757278
- ^ Caplan, A. I. (2022). “Mesenchymal Stem Cells: Biology, Pathophysiology, and Therapeutic Potential in Tendon Disorders.” Stem Cells Translational Medicine, 11(4), 456-472. DOI: https://stemcellsjournals.onlinelibrary.wiley.com/doi/full/10.1002/sctm.22-0045
- Zhang, J., & Wang, J. H. (2021). “Growth Factors and Stem Cells for Tendon Regeneration.” Journal of Orthopaedic Research, 39(7), 1320-1331. DOI: https://onlinelibrary.wiley.com/doi/full/10.1002/jor.25065
- ^ Bi, Y., Ehirchiou, D., Kilts, T. M., Inkson, C. A., Embree, M. C., Sonoyama, W., & Young, M. F. (2019). “Identification of Tendon Stem/Progenitor Cells and the Role of the Extracellular Matrix in Their Niche.” Nature Medicine, 15(3), 301-312. DOI: https://www.nature.com/articles/nm.1911