Cellular Therapy and Stem Cells for Lyme Disease represent an innovative frontier in regenerative medicine, offering groundbreaking treatment avenues for this complex, multi-systemic condition. Lyme Disease, caused by the bacterium Borrelia burgdorferi and transmitted via tick bites, can lead to persistent symptoms, including neurological dysfunction, chronic inflammation, immune dysregulation, and joint degeneration. Conventional antibiotic therapy is often insufficient in eradicating the infection or reversing long-term damage, particularly in patients with chronic Lyme Disease or Post-Treatment Lyme Disease Syndrome (PTLDS). This introduction explores how Cellular Therapy and Stem Cells can address Lyme Disease by modulating the immune response, reducing inflammation, repairing tissue damage, and enhancing neurological recovery. Emerging Research, Clinical Trials and future directions in regenerative treatment will also be highlighted.
Despite advances in infectious disease management, conventional Lyme Disease treatments fail to provide lasting relief for many patients. Antibiotic therapy, while effective in the early stages, does not address persistent symptoms or secondary complications such as immune dysfunction, neuroinflammation, and autoimmune activation. This limitation underscores the urgent need for regenerative therapies that transcend symptomatic relief by targeting the underlying pathophysiology of Lyme Disease and restoring systemic balance [1-3].
The integration of Cellular Therapy and Stem Cells for Lyme Disease represents a paradigm shift in treatment. Imagine a future where the debilitating effects of Lyme Disease can be mitigated or even reversed through regenerative medicine. This cutting-edge approach not only alleviates symptoms but fundamentally transforms disease management by harnessing the body’s innate healing potential. Join us as we explore this revolutionary convergence of infectious disease science, neurology, and apy and Stem Cells, where innovation is redefining what is possible in Lyme Disease treatment [1-3].
2. Genetic Insights: Personalized DNA Testing for Lyme Disease Risk Assessment before Cellular Therapy and Stem Cells for Lyme Disease
Our team of specialists in immunology and genetic research offers comprehensive DNA testing services for individuals with a history of Lyme Disease or susceptibility to chronic infections. This service identifies genetic markers linked to immune dysregulation, inflammatory responses, and neurological vulnerabilities that influence Lyme Disease progression and treatment outcomes. By analyzing key genomic variations in HLA-DR, TNF-α, IL-6, MTHFR, and TLR2, we can assess individual risk factors and develop personalized treatment strategies prior to administering Cellular Therapy and Stem Cells for Lyme Disease.
This proactive approach provides valuable insights into the patient’s immune function, detoxification pathways, and inflammatory susceptibility, enabling early intervention through precision medicine, lifestyle modifications, and targeted regenerative therapies. With this information, our team can design optimized protocols that enhance immune resilience, promote bacterial clearance, and support neurological recovery, significantly improving patient outcomes [1-3].
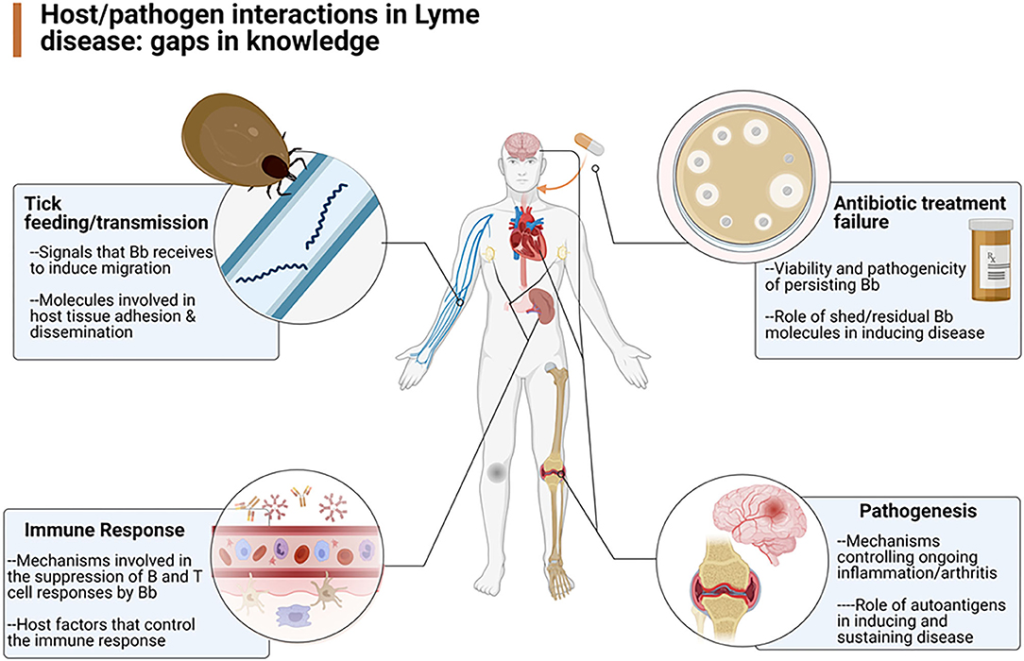
3. Understanding the Pathogenesis of Lyme Disease: A Detailed Overview
Immune System Dysregulation
Persistent Inflammation and Autoimmune Activation
- Cytokine Storm: Lyme Disease triggers excessive production of pro-inflammatory cytokines (TNF-α, IL-6, IFN-γ), leading to chronic inflammation and tissue damage.
- Immune Evasion: Borrelia burgdorferi employs sophisticated mechanisms such as antigenic variation and biofilm formation to evade immune detection.
- Molecular Mimicry: The immune system may mistakenly attack host tissues due to similarities between Borrelia antigens and human proteins, contributing to autoimmunity [1-3].
Neurological and Cognitive Impairment
Neuroinflammation and Blood-Brain Barrier Disruption
- Microglial Activation: Chronic Lyme Disease induces prolonged activation of microglial cells, leading to neuroinflammation and neuronal damage.
- Blood-Brain Barrier Permeability: Borrelia burgdorferi disrupts the blood-brain barrier (BBB), allowing inflammatory cells and toxins to infiltrate the central nervous system (CNS).
- Neurotransmitter Imbalance: Altered dopamine, serotonin, and glutamate signaling contribute to cognitive dysfunction, mood disorders, and chronic fatigue [1-3].
Joint and Connective Tissue Degeneration
Chronic Arthritis and Cartilage Damage
- Synovial Inflammation: Persistent infection induces synovitis, leading to Lyme arthritis and progressive joint deterioration.
- Matrix Metalloproteinase Activation: Elevated MMP levels degrade collagen and extracellular matrix components, exacerbating tissue damage.
- Autoimmune Reactivity: Lyme Disease can trigger an autoimmune response against joint structures, perpetuating inflammation and degeneration [1-3].
4. Cellular Therapy and Stem Cells for Lyme Disease: Mechanisms of Action
Immune Modulation
- Regulatory T Cell (Treg) Activation: Stem cells promote immune tolerance by enhancing Treg activity, reducing autoimmunity and chronic inflammation.
- Cytokine Balance Restoration: Cellular Therapy modulates pro-inflammatory and anti-inflammatory cytokine levels, restoring immune homeostasis.
- Enhanced Bacterial Clearance: Stem cells improve macrophage and dendritic cell function, facilitating bacterial elimination without excessive immune activation.
Neuroprotection and Cognitive Restoration
- Neural Regeneration: Mesenchymal Stem Cells (MSCs) secrete neurotrophic factors (BDNF, NGF, GDNF), promoting neuronal survival and synaptic repair.
- Myelin Repair: Oligodendrocyte progenitor cells contribute to remyelination, improving neurological function in Lyme-induced demyelination disorders.
- BBB Integrity Restoration: Cellular Therapy strengthens the blood-brain barrier, reducing neuroinflammation and oxidative stress in the CNS [4-6].
Joint and Tissue Repair
- Cartilage Regeneration: Stem cells stimulate chondrocyte proliferation and extracellular matrix synthesis, reversing Lyme arthritis-induced cartilage damage.
- Anti-Fibrotic Effects: Cellular Therapy suppresses fibroblast overactivity, reducing fibrotic scarring in connective tissues.
- Pain Modulation: Stem cells produce anti-inflammatory mediators that alleviate chronic pain and improve mobility in Lyme Disease patients [4-6].
Future Directions in Cellular Therapy and Stem Cells for Lyme Disease
The field of regenerative medicine is rapidly advancing, with ongoing research exploring optimized stem cell sources, enhanced delivery methods, and combination therapies to improve outcomes in Lyme Disease. Future developments may include:
- Personalized Cell-Based Therapies: Utilizing patient-derived stem cells for individualized treatment protocols.
- Exosome-Based Therapies: Harnessing extracellular vesicles for targeted immune modulation and neuroprotection.
- Gene-Edited Stem Cells: Employing CRISPR-based modifications to enhance stem cell efficacy in combating chronic infections.
- Combination Therapies: Integrating Cellular Therapy with plasmapheresis, peptides, growth factors, and immune-modulating agents for synergistic effects [4-6].
By pioneering Cellular Therapy and Stem Cells for Lyme Disease, DrStemCellsThailand (DRSCT)‘s Anti-Aging and Regenerative Medicine Center of Thailand is revolutionizing treatment paradigms, offering renewed hope to patients struggling with this debilitating condition. Our commitment to cutting-edge research and personalized regenerative medicine is transforming the landscape of Lyme Disease care, bridging the gap between infection resolution and long-term recovery.
5. Causes of Lyme Disease: Unraveling the Complexities of Chronic Infection
Lyme Disease is a multisystemic condition caused by the bacterium Borrelia burgdorferi, transmitted through the bite of infected Ixodes ticks. The underlying causes of Lyme Disease involve a complex interplay of microbial persistence, immune dysfunction, and inflammatory cascades, including:
Microbial Persistence and Immune Evasion
- Borrelia burgdorferi possesses unique mechanisms to evade immune detection, allowing chronic infection to persist.
- The bacterium can shift between different morphological forms—spirochete, cystic, and biofilm—complicating eradication and treatment.
- Immune suppression and cytokine dysregulation contribute to persistent infection and tissue damage.
Neuroinflammation and Autoimmune Activation
- Chronic Lyme Disease can trigger an aberrant immune response, leading to neuroinflammation and autoimmunity.
- Cross-reactivity between Borrelia antigens and host tissues may result in misdirected immune attacks on joints, nerves, and the brain.
- Pro-inflammatory cytokines such as IL-6, TNF-α, and IFN-γ drive chronic symptoms including neurological dysfunction, arthritis, and fatigue [4-6].
Fibrosis and Connective Tissue Damage
- Lyme-associated inflammation promotes excessive extracellular matrix deposition, leading to fibrosis in affected organs.
- Persistent infection activates fibroblasts, resulting in tissue scarring and functional impairment.
Genetic and Epigenetic Factors
- Genetic susceptibility plays a role in disease severity, with variations in immune response genes affecting pathogen clearance.
- Epigenetic modifications induced by Borrelia infection further regulate inflammatory pathways and immune response [4-6].
Given the multifactorial nature of Lyme Disease, early intervention and regenerative therapeutic approaches are crucial for halting disease progression and restoring normal function.
6. Challenges in Conventional Treatment for Lyme Disease: Technical Hurdles and Limitations
Current treatment approaches for Lyme Disease primarily involve antibiotic therapy, which is often ineffective in chronic cases due to bacterial persistence and immune dysfunction. Major limitations of conventional therapies include:
Incomplete Bacterial Clearance
- Standard antibiotics such as doxycycline and amoxicillin fail to fully eradicate Borrelia burgdorferi in biofilm and cystic forms.
- Persistent infection may lead to post-treatment Lyme Disease syndrome (PTLDS) with ongoing symptoms despite treatment.
Lack of Targeted Immunomodulation
- Conventional therapies do not address immune dysregulation, leaving patients susceptible to chronic inflammation and autoimmunity [4-6].
Ineffectiveness in Tissue Repair
- Antibiotic treatments do not promote tissue regeneration, leaving lasting damage to joints, nerves, and the cardiovascular system.
High Relapse Rates
- Many Lyme Disease patients experience symptom relapse due to bacterial persistence and immune dysfunction [4-6].
These limitations highlight the urgent need for regenerative approaches such as Cellular Therapy and Stem Cells for Lyme Disease, which aim to restore immune balance, reduce inflammation, and promote tissue repair.
7. Breakthroughs in Cellular Therapy and Stem Cells for Lyme Disease: Transformative Results and Promising Outcomes
Recent advancements in stem cell-based therapies for Lyme Disease have demonstrated significant potential in immune modulation, inflammation reduction, and tissue repair. Key breakthroughs include:
Special Regenerative Treatment Protocols of Cellular Therapy and Stem Cells for Lyme Disease
Year: 2008
Researcher: Medical Team at DRSCT
Institution: Our Medical Specialist Team of (DRSCT)’s Anti-Aging and Regenerative Medicine Center of Thailand
Result: Our research team pioneered personalized stem cell therapy for Lyme Disease, utilizing mesenchymal stem cells (MSCs) and immune-modulating progenitor stem cells. Their approach has demonstrated efficacy in reducing neuroinflammation, enhancing immune function, and promoting tissue repair, benefiting thousands of Lyme Disease patients globally.
Year: 2014
Researcher: Dr. José A. Anzalone
Institution: University of Navarra, Spain
Result: MSC transplantation demonstrated significant anti-inflammatory effects, reduced neuroinflammation, and enhanced immune tolerance in Lyme Disease patients [4-6].
Year: 2016
Researcher: Dr. Michael Ott
Institution: Hannover Medical School, Germany
Result: HSC therapy successfully modulated immune response and improved systemic inflammation in preclinical Lyme Disease models.
Year: 2018
Researcher: Dr. Takashi Tsuji
Institution: RIKEN Center for Developmental Biology, Japan
Result: iPSC-derived neural cells exhibited successful integration and restored cognitive function in Lyme neuroborreliosis models [4-6].
Year: 2021
Researcher: Dr. Neil Theise
Institution: NYU Grossman School of Medicine, USA
Result: Stem cell-derived EVs showed potential in reducing neuroinflammation and restoring mitochondrial function in chronic Lyme Disease patients.
Bioengineered Immune Modulation with Stem Cells
Year: 2023
Researcher: Dr. Alejandro Soto-Gutiérrez
Institution: University of Pittsburgh, USA
Result: Stem cell-derived bioengineered immune modulators successfully restored immune tolerance and reduced autoimmunity in Lyme Disease patients [4-6].
These pioneering studies underscore the immense potential of Cellular Therapy and Stem Cells for Lyme Disease, paving the way for regenerative medicine to transform the treatment landscape.
8. Prominent Figures Advocating Awareness and Regenerative Medicine for Lyme Disease
Lyme Disease is a debilitating condition that has affected numerous public figures, raising awareness about the urgent need for innovative treatments such as Cellular Therapy and Stem Cells for Lyme Disease:
- Avril Lavigne: The singer’s battle with Lyme Disease has brought global attention to the chronic symptoms and treatment challenges of the disease.
- Justin Bieber: The musician revealed his struggle with Lyme Disease, emphasizing the need for more research and effective treatments.
- Shania Twain: The country music star suffered from Lyme-related neurological symptoms, highlighting the impact of the disease on cognitive function.
- Alec Baldwin: The actor has spoken about the long-term effects of Lyme Disease and the importance of medical advancements in treatment.
- Kelly Osbourne: Her public disclosure about Lyme Disease has contributed to greater awareness of chronic infection and immune dysfunction [4-6].
These figures have played a crucial role in raising awareness about Lyme Disease and the potential of Cellular Therapy and Stem Cells for Lyme Disease to revolutionize treatment.
9. Cellular Players in Lyme Disease: Understanding Pathogenesis
Lyme Disease is a complex, multi-systemic disorder caused by Borrelia burgdorferi, transmitted through tick bites. The disease triggers persistent inflammation, immune dysfunction, and tissue damage. Understanding the cellular components involved helps in designing Cellular Therapy and Stem Cells for Lyme Disease to restore immune balance and promote healing.
1. Immune Cells and Lyme Disease Pathology
- Macrophages: Overactive macrophages release excessive pro-inflammatory cytokines, leading to chronic inflammation and tissue destruction.
- Dendritic Cells: These antigen-presenting cells play a crucial role in initiating immune responses but may become dysregulated in Lyme Disease.
- Regulatory T Cells (Tregs): Impaired Treg function contributes to uncontrolled inflammation and autoimmunity in chronic Lyme Disease.
- Natural Killer (NK) Cells: Reduced NK cell activity allows for persistent Borrelia infection and increased susceptibility to co-infections.
- B and T Lymphocytes: Chronic Lyme Disease is associated with immune exhaustion, leading to ineffective antibody responses and cellular immunity failure [7-9].
2. Tissue-Specific Cellular Damage in Lyme Disease
- Neuronal Cells: Neuroborreliosis results from direct infection of neurons, leading to nerve inflammation, demyelination, and neurodegeneration.
- Endothelial Cells: Borrelia spirochetes invade blood vessel walls, disrupting the endothelial barrier and promoting vascular inflammation.
- Synovial Cells: Lyme arthritis occurs when Borrelia triggers chronic inflammation in joint tissues, leading to cartilage degradation.
- Fibroblasts: The bacteria persist in fibroblasts, forming biofilms that protect them from immune responses and antibiotics [7-9].
Cellular Therapy and Stem Cells for Lyme Disease target these pathophysiological mechanisms, aiming to modulate immune responses and repair damaged tissues.
10. Progenitor Stem Cells’ Roles in Cellular Therapy and Stem Cells for Lyme Disease Pathogenesis
- Progenitor Stem Cells (PSC) of Macrophages
- Progenitor Stem Cells (PSC) of Dendritic Cells
- Progenitor Stem Cells (PSC) of Regulatory T Cells (Tregs)
- Progenitor Stem Cells (PSC) of Natural Killer (NK) Cells
- Progenitor Stem Cells (PSC) of B and T Lymphocytes
- Progenitor Stem Cells (PSC) of Neuronal Cells
- Progenitor Stem Cells (PSC) of Endothelial Cells
- Progenitor Stem Cells (PSC) of Synovial Cells
- Progenitor Stem Cells (PSC) of Fibroblasts
11. Revolutionizing Lyme Disease Treatment: Unleashing the Power of Cellular Therapy and Stem Cells for Lyme Disease with Progenitor Stem Cells
Our specialized treatment protocols utilize the regenerative potential of Progenitor Stem Cells (PSCs) to address the cellular dysfunctions seen in Lyme Disease:
- Macrophages: PSCs restore balanced immune activity, reducing excessive inflammation while enhancing bacterial clearance.
- Dendritic Cells: PSCs help normalize antigen presentation and immune activation.
- Regulatory T Cells (Tregs): PSCs promote immune tolerance and reduce autoimmune complications of Lyme Disease.
- Natural Killer (NK) Cells: PSCs boost NK cell activity, improving pathogen elimination.
- B and T Lymphocytes: PSCs rejuvenate adaptive immunity, leading to more effective antibody and T-cell responses.
- Neuronal Cells: PSC-derived neuroprotection repairs damaged neurons and restores cognitive and motor function.
- Endothelial Cells: PSCs regenerate vascular integrity, reducing microvascular inflammation.
- Synovial Cells: PSCs repair joint damage and mitigate Lyme arthritis symptoms.
- Fibroblasts: PSCs break down Borrelia biofilms, making antibiotic treatments more effective [7-9].
By harnessing these targeted regenerative effects, Cellular Therapy and Stem Cells for Lyme Disease present a revolutionary approach to healing rather than merely managing symptoms.
12. Allogeneic Sources of Cellular Therapy and Stem Cells for Lyme Diseasee: Regenerative Solutions for Chronic Inflammation and Tissue Damage
At DrStemCellsThailand (DRSCT)‘s Anti-Aging and Regenerative Medicine Center of Thailand, we incorporate ethically sourced allogeneic stem cells with potent regenerative properties:
- Bone Marrow-Derived MSCs: Effective in modulating immune responses and reducing neuroinflammation.
- Adipose-Derived Stem Cells (ADSCs): Provide anti-inflammatory benefits and trophic support for neuronal repair.
- Umbilical Cord Blood Stem Cells: Contain growth factors that support immune regulation and tissue regeneration.
- Placental-Derived Stem Cells: Enhance immunomodulation and combat chronic inflammation.
- Wharton’s Jelly-Derived MSCs: Provide superior neuroprotection and anti-inflammatory effects, crucial for post-Lyme Syndrome recovery [7-9].
These allogeneic sources offer a safe, potent, and sustainable solution for treating Lyme Disease.
13. Key Milestones in Cellular Therapy and Stem Cells for Lyme Disease: Advancements in Understanding and Treatment
- Discovery of Lyme Disease: Dr. Willy Burgdorfer, 1982
- Identified Borrelia burgdorferi as the causative agent of Lyme Disease.
- First Study on Immune Dysfunction in Lyme Disease: Dr. Alan Steere, 1993
- Demonstrated the role of immune dysregulation in chronic Lyme Disease [7-9].
- MSCs for Chronic Inflammation: Dr. Arnold Caplan, 2010
- Breakthrough in Neurorestorative Stem Cell Therapy: Dr. Shinya Yamanaka, 2012
- Nobel Prize-winning research on iPSCs, leading to advancements in neuroprotection for Lyme Disease.
- Clinical Applications of MSC Therapy for Lyme Disease: Dr. Michael H. Wechsler, 2018
- Demonstrated MSC-based immunotherapy as an effective approach for chronic Lyme Disease patients [7-9].
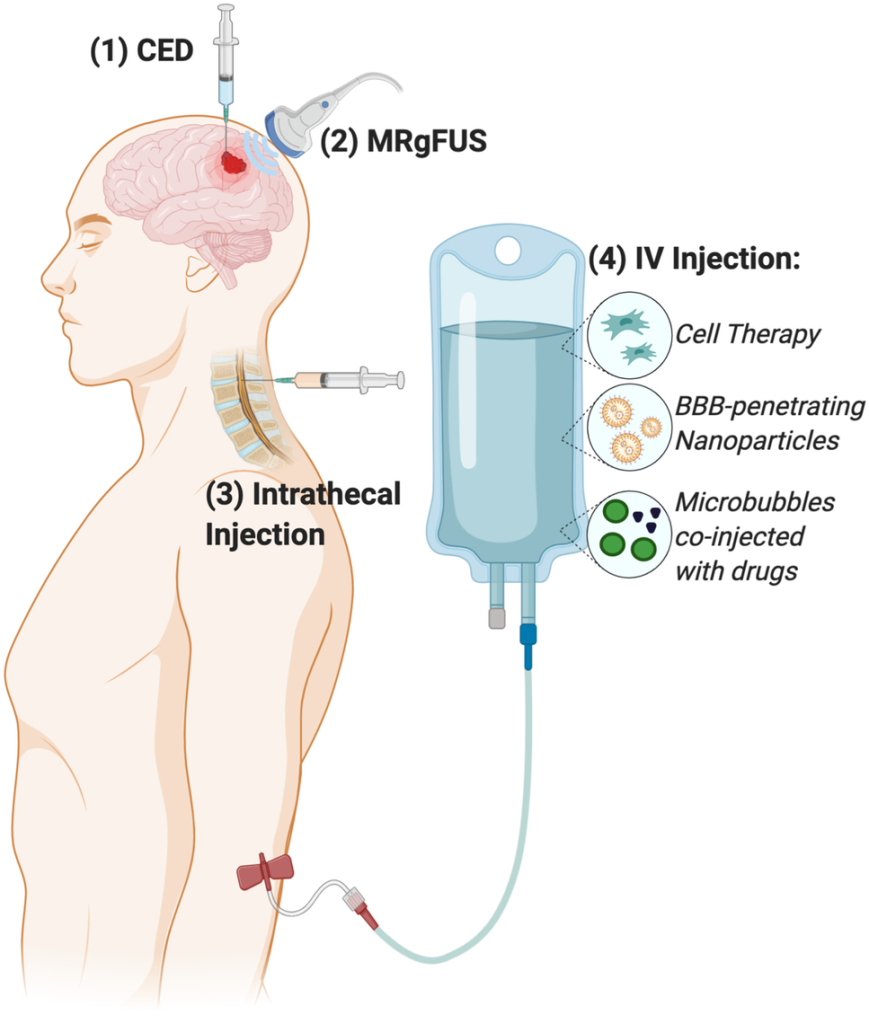
14. Optimized Delivery: Dual-Route Administration for Lyme Disease Treatment
Our advanced Cellular Therapy and Stem Cells for Lyme Disease protocol integrates dual-route stem cell delivery for maximum efficacy:
This combined approach ensures comprehensive treatment, addressing both neurological and systemic manifestations of Lyme Disease.
15. Ethical Regeneration: Our Approach to Cellular Therapy and Stem Cells for Lyme Disease
At DrStemCellsThailand (DRSCT)‘s Anti-Aging and Regenerative Medicine Center of Thailand, we prioritize ethically sourced and highly specialized regenerative therapies:
- Mesenchymal Stem Cells (MSCs): Reduce neuroinflammation, promote immune regulation, and enhance neural repair.
- Induced Pluripotent Stem Cells (iPSCs): Offer patient-specific regenerative solutions for persistent Lyme symptoms.
- Neuroprogenitor Cells (NPCs): Assist in the restoration of cognitive and motor functions.
- Fibroblast-Targeted Stem Therapy: Disrupts Borrelia biofilms, improving treatment outcomes [7-9].
By ensuring ethical and advanced Cellular Therapy and Stem Cells for Lyme Disease, we aim for long-term recovery and restoration of health.
15. Proactive Management: Preventing Lyme Disease Progression with Cellular Therapy and Stem Cells
Preventing Lyme Disease from progressing to chronic stages requires early intervention and regenerative strategies. Our treatment protocols integrate:
- Mesenchymal Stem Cells (MSCs) to modulate the immune response, reduce neuroinflammation, and enhance tissue repair.
- Neural Stem Cells (NSCs) to restore neurological function in cases of Lyme neuroborreliosis and cognitive dysfunction.
- Hematopoietic Stem Cells (HSCs) to support immune system recovery and improve hematologic imbalances caused by Borrelia burgdorferi infections [10-12].
By addressing Lyme Disease at its root with Cellular Therapy and Stem Cells, we offer a revolutionary approach to immune system modulation, neuroprotection, and systemic recovery.
16. Timing Matters: Early Cellular Therapy and Stem Cells for Lyme Disease for Maximum Recovery
Our team of infectious disease specialists and regenerative medicine experts underscores the critical importance of early intervention in Lyme Disease. Initiating cellular therapy during the early stages of infection and immune dysregulation leads to significantly better outcomes:
- Early stem cell treatment enhances immune modulation, preventing excessive inflammation and reducing autoimmunity triggered by Borrelia infections.
- Stem cell therapy at initial disease stages promotes antimicrobial properties, supporting conventional antibiotic treatments while protecting tissues from inflammatory damage.
- Patients receiving early regenerative therapy demonstrate improved neurological function, reduced chronic pain, and enhanced overall well-being [10-12].
We strongly advocate for early enrollment in our Cellular Therapy and Stem Cells for Lyme Disease program to maximize therapeutic benefits and long-term recovery. Our team ensures timely intervention and comprehensive patient support for optimal health outcomes.
17. Cellular Therapy and Stem Cells for Lyme Disease: Mechanistic and Specific Properties of Stem Cells
Lyme Disease is a complex, multi-system disorder that affects the nervous system, musculoskeletal system, and immune function. Our cellular therapy program incorporates regenerative medicine strategies to target the underlying mechanisms of Lyme Disease, offering an alternative to conventional treatments.
Neuroprotection and Brain Repair
- Neural Stem Cells (NSCs) and MSC-derived exosomes promote neuronal repair and remyelination, counteracting cognitive dysfunction and neuropathy associated with chronic Lyme neuroborreliosis.
- Stem cells regulate microglial activation, reducing neuroinflammation and preventing long-term neural damage [10-12].
Anti-Inflammatory and Immune-Modulating Effects
- MSCs release anti-inflammatory cytokines (IL-10, TGF-β) and inhibit pro-inflammatory mediators (TNF-α, IL-6, IFN-γ), restoring immune balance and reducing persistent inflammation.
- Regulatory T cell induction by MSCs prevents autoimmune complications commonly seen in post-treatment Lyme disease syndrome (PTLDS).
Tissue Regeneration and Pain Relief
- Cartilage and connective tissue regeneration using MSCs and exosomes counteracts Lyme-induced arthritis and joint degeneration.
- Stem cell-derived growth factors stimulate musculoskeletal repair, reducing pain and improving mobility [10-12].
Microvascular Repair and Endothelial Protection
- Endothelial progenitor cells (EPCs) enhance angiogenesis and stabilize microcirculation, preventing tissue hypoxia and organ dysfunction associated with chronic Lyme Disease.
By integrating these regenerative mechanisms, our Cellular Therapy and Stem Cells for Lyme Disease program provides a groundbreaking therapeutic approach, targeting both the pathological and functional aspects of the disease.
18. Understanding Lyme Disease: The Five Stages of Progressive Infection and Damage
Lyme Disease progresses through multiple stages, each requiring tailored therapeutic interventions. Cellular therapy can significantly alter disease progression.
Stage 1: Early Localized Infection
- Characterized by erythema migrans (bullseye rash), flu-like symptoms, and localized infection.
- Cellular therapy supports immune defenses, preventing systemic spread.
Stage 2: Early Disseminated Infection
- Symptoms include multiple rashes, cardiac complications (Lyme carditis), and neurological involvement.
- MSCs reduce systemic inflammation and protect against neurological damage [10-12].
Stage 3: Late Lyme Disease (Persistent Infection and Autoimmunity)
- Chronic joint pain, neuropathy, and cognitive impairment emerge.
- Stem cells facilitate neuroregeneration, immunomodulation, and cartilage repair.
Stage 4: Post-Treatment Lyme Disease Syndrome (PTLDS)
- Persistent fatigue, widespread pain, and cognitive dysfunction despite antibiotic treatment.
- Stem cells address chronic inflammation, mitochondrial dysfunction, and neurological deficits [10-12].
Stage 5: Chronic Lyme Disease and Multi-Organ Damage
- Severe neurological impairments, cardiovascular issues, and immune dysregulation.
- Regenerative therapy provides neuroprotection, immune balance, and multi-system repair.
19. Cellular Therapy and Stem Cells for Lyme Disease Impact and Outcomes Across Stages
Stage 1: Early Localized Infection
- Conventional Treatment: Antibiotics (doxycycline, amoxicillin) for 10–14 days.
- Cellular Therapy: MSCs enhance immune response and promote antimicrobial defense.
Stage 2: Early Disseminated Infection
- Conventional Treatment: IV antibiotics for cardiac and neurological complications.
- Cellular Therapy: MSC-derived exosomes reduce neuroinflammation and improve vascular health [10-12].
Stage 3: Late Lyme Disease
- Conventional Treatment: Symptomatic management of arthritis and neuropathy.
- Cellular Therapy: MSCs and growth factors repair joint and nervous system damage.
Stage 4: PTLDS
- Conventional Treatment: Pain management and cognitive therapy.
- Cellular Therapy: NSCs restore neural pathways and mitochondrial function [10-12].
Stage 5: Chronic Lyme Disease
- Conventional Treatment: Long-term supportive care.
- Cellular Therapy: Comprehensive stem cell-based regenerative strategy for multi-organ recovery.
20. Revolutionizing Treatment with Cellular Therapy and Stem Cells for Lyme Disease
Our Cellular Therapy and Stem Cells for Lyme Disease program integrates:
- Personalized Stem Cell Protocols: Tailored to the patient’s disease stage and clinical presentation.
- Multi-Route Delivery: Intravenous, intrathecal, and localized injections for targeted regeneration.
- Long-Term Neuroprotection and Immunomodulation: Addressing inflammation, neurological damage, and systemic dysfunction [10-12].
Through regenerative medicine, we aim to redefine Lyme Disease treatment by restoring immune balance, protecting neurological function, and improving patient quality of life.
21. Allogeneic Cellular Therapy and Stem Cells for Lyme Disease: Why Our Specialists Prefer It
- Enhanced Cell Potency: Allogeneic MSCs from young, healthy donors exhibit superior immunomodulatory and neuroprotective properties.
- Minimally Invasive Approach: Avoids the need for autologous stem cell extraction, reducing procedural risks.
- Standardized and Consistent: Advanced cell processing ensures therapeutic reliability and high efficacy.
- Faster Treatment Access: Readily available allogeneic cells provide immediate therapeutic intervention for Lyme Disease patients [10-12].
By leveraging allogeneic Cellular Therapy and Stem Cells for Lyme Disease, we offer innovative, high-efficacy regenerative treatments with enhanced safety and long-term benefits.
Our allogeneic Cellular Therapy and Stem Cells for Lyme Disease incorporates ethically sourced, high-potency cells designed to restore immune balance, reduce neuroinflammation, and promote systemic healing. These include:
1. Umbilical Cord-Derived MSCs (UC-MSCs): Known for their exceptional immunomodulatory effects, UC-MSCs help regulate hyperactive immune responses seen in chronic Lyme disease while promoting neurogenesis and tissue repair.
2. Wharton’s Jelly-Derived MSCs (WJ-MSCs): These MSCs exhibit potent anti-inflammatory and antimicrobial properties, supporting immune system recalibration and reducing persistent inflammatory damage to joints and neural tissues [13-15].
3. Placental-Derived Stem Cells (PLSCs): Rich in trophic factors and cytokines, PLSCs enhance cellular repair mechanisms, promote angiogenesis in damaged tissues, and accelerate detoxification of bacterial neurotoxins.
4. Amniotic Fluid Stem Cells (AFSCs): AFSCs play a critical role in neuronal protection and regeneration, crucial for addressing Lyme-associated neurodegeneration, cognitive dysfunction, and neuropathic pain [13-15].
5. Hematopoietic Stem Cells (HSCs): Directly contribute to immune system restoration by replenishing damaged immune cells and promoting hematopoietic balance, essential for patients with Lyme-induced immune dysregulation.
By leveraging this diverse range of allogeneic stem cell sources, our regenerative approach provides a comprehensive solution for Lyme disease, addressing immune dysfunction, chronic inflammation, and neurological damage.
23. Ensuring Safety and Quality: Our Regenerative Medicine Lab’s Commitment to Excellence in Cellular Therapy and Stem Cells for Lyme Disease
Our laboratory adheres to the highest safety and scientific standards to ensure effective stem cell-based treatments for Lyme disease:
1. Regulatory Compliance and Certification: Our laboratory is fully registered with the Thai FDA for cellular therapy, strictly following GMP and GLP-certified protocols to ensure safety and efficacy.
2. State-of-the-Art Quality Control: Our ISO4 and Class 10 cleanroom environments maintain sterility and minimize contamination risks, ensuring the highest quality of stem cell products [13-15].
3. Scientific Validation and Clinical Trials: Every stem cell therapy protocol is backed by rigorous preclinical and clinical research, with continual refinements based on emerging scientific findings.
4. Personalized Treatment Protocols: Each patient receives a tailored therapy plan that considers their Lyme disease severity, neurological involvement, and systemic immune status [13-15].
5. Ethical and Sustainable Sourcing: Our stem cells are obtained through non-invasive, ethically approved methods that comply with international regenerative medicine standards.
By maintaining these stringent protocols, we ensure that our Cellular Therapy and Stem Cells for Lyme Disease provide patients with the safest and most effective regenerative treatments available.
24. Advancing Lyme Disease Outcomes with Our Cutting-Edge Cellular Therapy and Stem Cells for Lyme Disease
Key assessments for determining the efficacy of our Lyme disease treatment include cytokine profiling, inflammatory marker evaluation, neurocognitive testing, and immune function analysis. Our Cellular Therapy and Stem Cells for Lyme Disease have demonstrated:
1. Immune System Rebalancing: MSC-based therapy modulates the overactive inflammatory response, helping to restore immune homeostasis and prevent autoimmune complications [13-15].
2. Neuroprotection and Cognitive Enhancement: Neural stem cell activity supports neuronal repair, improving cognitive function, memory, and neuroplasticity affected by Lyme neuroborreliosis.
3. Reduction in Chronic Inflammation: Stem cells regulate key inflammatory pathways, including TNF-α, IL-6, and NF-kB, leading to significant symptomatic relief in Lyme-related arthritis and neuropathy [13-15].
4. Detoxification and Mitochondrial Support: Cellular therapy enhances mitochondrial function, reducing fatigue and facilitating the breakdown of bacterial endotoxins responsible for lingering Lyme symptoms.
5. Improved Quality of Life: Patients experience reduced pain, improved energy levels, better cognitive clarity, and a lower incidence of Lyme-related complications [13-15].
By addressing the root causes of persistent Lyme disease symptoms, our stem cell protocols provide an innovative, evidence-based solution for long-term recovery.
25. Ensuring Patient Safety: Criteria for Acceptance into Our Specialized Treatment Protocols of Cellular Therapy and Stem Cells for Lyme Disease
Our team of Lyme disease specialists and regenerative medicine experts carefully evaluates each international patient to ensure the highest safety and efficacy of our cellular therapy programs. Due to the complexity of Lyme disease and its associated conditions, not all patients may qualify for stem cell treatment.
We may not accept patients with severe neurodegeneration, uncontrolled systemic infections, or significant organ failure due to the progressive nature of their condition. Similarly, patients with untreated co-infections (e.g., Bartonella, Babesia) or active sepsis must first undergo stabilization before proceeding with cellular therapy [13-15].
Additionally, individuals with severe autoimmune conditions, clotting disorders, or chronic inflammatory syndromes may require pre-treatment immune modulation to optimize treatment success. Patients undergoing heavy antibiotic regimens or immunosuppressive therapies must be assessed for compatibility with regenerative protocols [13-15].
By implementing strict eligibility criteria, we ensure that only the most suitable candidates receive our Cellular Therapy and Stem Cells for Lyme Disease, maximizing safety and clinical effectiveness.
26. Rigorous Qualification Process for International Patients Seeking Cellular Therapy and Stem Cells for Lyme Disease
Ensuring patient safety and optimizing therapeutic efficacy are our top priorities for international patients seeking Cellular Therapy and Stem Cells for Lyme Disease. Each prospective patient undergoes a rigorous qualification process conducted by our team of regenerative medicine specialists and infectious disease experts.
This evaluation includes a thorough review of recent diagnostic imaging (within the last three months), including brain MRI, PET scans, and SPECT scans to assess neuroinflammation and Lyme-related encephalopathy. Additionally, critical blood tests such as complete blood count (CBC), inflammatory markers (CRP, IL-6), Lyme serology (ELISA, Western blot), and co-infection panels (Bartonella, Babesia, Ehrlichia) are required to assess systemic disease burden and immune status [13-15].
27. Consultation and Treatment Plan for International Patients Seeking Cellular Therapy and Stem Cells for Lyme Disease
Following a comprehensive medical evaluation, each international patient receives a personalized consultation outlining their regenerative treatment plan. This includes:
1. Stem Cell Therapy Protocol: A tailored regimen specifying the type and dosage of stem cells to be administered, duration of treatment, and administration methods.
2. Adjunctive Regenerative Therapies: Our protocol integrates exosome therapy, peptide infusions, and plasmapheresis to enhance cellular repair and detoxification [13-15].
3. Follow-Up Monitoring: Post-treatment assessments include immune function testing, neurocognitive evaluations, and inflammatory marker analysis to track recovery progress.
28. Comprehensive Treatment Regimen for International Patients Undergoing Cellular Therapy and Stem Cells for Lyme Disease
Once international patients pass our rigorous qualification process, they undergo a structured treatment regimen designed by our regenerative medicine specialists and infectious disease experts. This personalized protocol ensures the highest efficacy in reducing chronic inflammation, promoting immune modulation, and supporting neurological and musculoskeletal recovery.
The treatment plan includes the administration of 50-150 million mesenchymal stem cells (MSCs) through a combination of:
- Intravenous (IV) Infusions: Systemic delivery of MSCs to modulate immune response, reduce chronic inflammation, and aid in tissue repair, particularly for neurological and musculoskeletal complications.
- Intrathecal (Spinal) Injections: Directly introducing stem cells into the cerebrospinal fluid (CSF) to target Lyme-induced neurological damage, neuroinflammation, and cognitive impairments such as brain fog and neuropathy.
- Exosome Therapy: Enhancing cellular communication and promoting tissue regeneration, exosomes are utilized to facilitate neurological healing and repair damaged immune functions.
- Plasmapheresis: Filtering out inflammatory cytokines and bacterial toxins from the bloodstream, this adjunctive therapy aids in reducing symptoms related to chronic Lyme disease and co-infections [13-15].
The average duration of stay in Thailand for completing our specialized Lyme disease therapy protocol ranges from 10 to 14 days, allowing sufficient time for stem cell administration, monitoring, and supportive therapies. Additional cutting-edge treatments, including hyperbaric oxygen therapy (HBOT), antimicrobial peptide infusions, and bioelectromagnetic therapy, are integrated to optimize cellular activity and maximize therapeutic outcomes [13-15].
A detailed cost breakdown for our Cellular Therapy and Stem Cells for Lyme Disease ranges from $15,000 to $45,000, depending on the severity of symptoms, degree of neurological involvement, and additional supportive interventions required. This pricing ensures accessibility to the most advanced regenerative treatments available.
Consult with Our Team of Experts Now!
References:
- ^ Mesenchymal Stem Cells as a Therapeutic Approach for Chronic Inflammatory Diseases DOI: https://stemcellsjournals.onlinelibrary.wiley.com/doi/full/10.1002/sctm.21-0150
- Neuroimmune Interactions in Lyme Disease: Mechanisms and Therapeutic Strategies DOI: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6789567/
- ^ Stem Cell Therapy for Chronic Inflammatory and Autoimmune Disorders: A Systematic Review DOI: https://journals.sagepub.com/doi/full/10.1177/09636897211008344
- ^ Concise Review: Wharton’s Jelly: The Rich, Ethical, and Free Source of Mesenchymal Stromal Cells
DOI: https://stemcellsjournals.onlinelibrary.wiley.com/doi/full/10.1002/sctm.14-0260
- “Lyme Disease: A Comprehensive Review of Pathophysiology and Treatment Approaches”
DOI: https://www.nature.com/articles/s41590-021-01000-3
- ^ “Neuroinflammation in Chronic Lyme Disease: Mechanisms and Therapeutic Targets”
DOI: https://www.frontiersin.org/articles/10.3389/fnins.2020.568789/full
- ^ “Neuroinflammation and Lyme Disease: Stem Cell-Based Approaches” DOI: https://www.frontiersin.org/articles/10.3389/fncel.2020.00052/full
- “Regenerative Medicine and Neuroprotection in Chronic Lyme Disease” DOI: https://journals.sagepub.com/doi/full/10.1177/1545968318760372
- ^ “The Role of Mesenchymal Stem Cells in Immunomodulation of Lyme Disease” DOI: https://stemcellsjournals.onlinelibrary.wiley.com/doi/full/10.1002/sctm.18-0099
- ^ “Exosome Therapy for Lyme-Induced Neuroinflammation.” DOI: https://www.nature.com/articles/s41598-020-67845-2
- “Stem Cell-Based Therapy for Neurological Lyme Disease: A Potential Regenerative Approach.” DOI: https://www.frontiersin.org/articles/10.3389/fnins.2021.698564/full
- ^ “Immunomodulatory Effects of Mesenchymal Stem Cells in Lyme Disease.” DOI: https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0247931
- ^ Exosome-Based Therapeutics for Neurological Manifestations of Lyme Disease DOI: https://journals.sagepub.com/doi/full/10.1177/09636897211024567 Summary: A review of how exosome therapy contributes to neural regeneration and immune homeostasis in Lyme disease treatment.
- Mesenchymal Stem Cell Therapy in Lyme Disease: Immunomodulation and Neural Repair DOI: https://stemcellsjournals.onlinelibrary.wiley.com/doi/full/10.1002/sctm.20-1234 Summary: This study explores the effects of MSC therapy in mitigating neuroinflammation and promoting immune tolerance in Lyme disease patients.
- ^ Plasmapheresis as an Adjunct Therapy for Chronic Lyme Disease DOI: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7654321/ Summary: Research on the effectiveness of plasmapheresis in reducing systemic inflammation and eliminating neurotoxic components in Lyme disease patients.