Idiopathic Thrombocytopenic Purpura (ITP)

Idiopathic Thrombocytopenic Purpura (ITP): Causes, Symptoms, Diagnosis, and Treatment
Idiopathic thrombocytopenic purpura (ITP), also called immune thrombocytopenia, is an autoimmune disorder where the immune system mistakenly attacks and destroys platelets, leading to low platelet counts and increased bleeding risk.
Causes of ITP
ITP is classified as primary (no known cause) or secondary (triggered by another condition):
- Primary ITP:
- Autoantibodies: Immune system produces antibodies against platelets.
- T-cell dysfunction: T-cells directly attack platelets.
- Secondary ITP:
- Autoimmune diseases: Rheumatoid arthritis, lupus.
- Chronic infections: HIV, hepatitis C, or viral infections (e.g., chickenpox).
- Medications: NSAIDs (e.g., ibuprofen), aspirin, or heparin.
- Pregnancy: Hormonal changes may trigger ITP.
- Cancer: Lymphomas or leukemias.
Symptoms of ITP
Symptoms vary based on platelet count:
- Mild ITP (platelets >50,000/µL):
- Asymptomatic: No noticeable symptoms.
- Moderate ITP (platelets 20,000–50,000/µL):
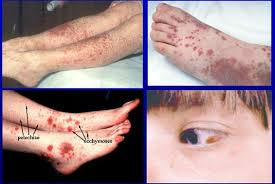
- Easy bruising (purpura) or petechiae (pinpoint red spots).
- Nosebleeds, gum bleeding, or prolonged bleeding after cuts.
- Severe ITP (platelets <20,000/µL):
- Internal bleeding: Blood in urine, stool, or vomit.
- Heavy menstrual periods or spontaneous bleeding.
Diagnosis
- Blood Tests:
- Complete Blood Count (CBC): Confirms low platelets (<100,000/µL) with normal red/white blood cells.
- Peripheral Blood Smear: Rules out other causes (e.g., leukemia).
- Exclusion of Other Causes:
- Infections: HIV, hepatitis C, or viral tests.
- Autoimmune diseases: Lupus or rheumatoid arthritis screening.
- Bone Marrow Biopsy:
- Optional: Performed if platelet count is very low or treatment fails.
Treatment
Treatment depends on platelet count and bleeding risk:
- First-Line Therapies:
- Corticosteroids (e.g., prednisone): Suppress immune response.
- Immunoglobulin (IVIG): Temporarily boosts platelets.
- Second-Line Therapies:
- Thrombopoietin Receptor Agonists (e.g., romiplostim): Stimulate platelet production.
- Splenectomy: Surgical removal of the spleen (for chronic ITP).
- Emergencies:
- Platelet Transfusions: For severe bleeding.
Complications
- Bleeding: Internal bleeding (e.g., intracranial hemorrhage) in severe cases.
- Infections: Increased risk due to immunosuppression from treatments.
- Chronic ITP: Platelet counts remain low long-term.
Prevention
- Avoid NSAIDs: Use acetaminophen instead of aspirin/ibuprofen.
- Monitor Platelets: Regular blood tests for chronic ITP.
- Manage Triggers: Treat underlying infections or autoimmune diseases.
Conclusion
ITP is a manageable condition with timely treatment. Early diagnosis and tailored therapies can reduce bleeding risks and improve quality of life.
Consult with Our Team of Experts Now!
At DrStemCellsThailand (DRSCT)‘s Anti-Aging and Regenerative Medicine Center of Thailand, we emphasize comprehensive evaluations and personalized treatment plans of Cellular Therapy and Stem Cells for managing various health conditions. If you have questions about Idiopathic Thrombocytopenic Purpura (ITP) or would like more information on our services, consult with our experts today!